Catching COVID-19 twice: Does it happen and what are the implications?
"If the viral DNA sequence between the two tests is the same or very similar, this indicates that the patient has not really removed the virus," said Dr. Labzin
- by B2B Desk 2020-07-24 06:52:23
Some reports from around the world about patients who appear to have been infected with the second coronavirus might be worrying, but experts say it's too early to jump to conclusions.
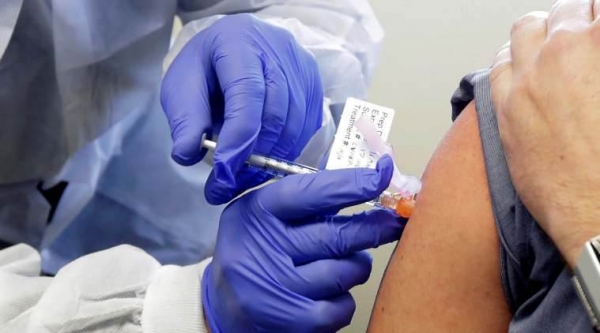
Earlier this month, a Washington DC doctor reported on a 50-year-old patient who had been diagnosed with the SARS-CoV-2, the virus that causes COVID-19, three months after his first infection.
Instead of having just a mild cough and sore throat as it did the first time, the second infection was worse and included severe fever, shortness of breath, and many trips to the hospital.
Or worse, COVID could be like dengue fever where you get sick when you get an infection again.
Dr. Ackerly wrote: "It is also troubling that a patient's condition, and other conditions such as his, may cloud hope for natural herd immunity."
Herd immunity is the place where a sufficient number of people are exposed to viral proteins, either naturally or from a vaccine, to develop immunity and stop the spread of the virus.
How sure are we these are cases of reinfection?
There were also several cases of sick people who had been documented a second time in France, but we were still unable to confirm what was happening in these isolated reports, said Larisa Labzin, a specialist in viral immunity at the University of Queensland.
"There are no scientifically reviewed peer-reviewed studies that have definitively demonstrated a return of infection," said Dr. Labzen.
"There is only anecdotal evidence from the United States and other countries."

It is possible that these second diseases are caused by the original virus, which was not eliminated from the body after the first illness, Dr. Labzen said.
This can happen, for example, when the virus level temporarily drops below the detection capacity of the test, leading to a "false negative" result.
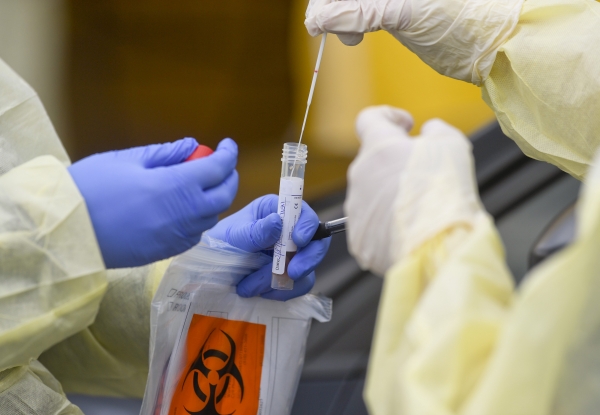
To find out if this is the case, the genetic material of the virus (RNA) should be serialized in each of the coronavirus tests that were performed during the first and second diseases.
"If the viral DNA sequence between the two tests is the same or very similar, this indicates that the patient has not really removed the virus," said Dr. Labzin.
"If the sequence of the virus is very different, we can make sure that it has already returned to infection."
But Dr. Labzin said that this type of sequencing has not yet occurred again in cases of infection, so we cannot exclude this possibility.
If reinfections happen, how common is getting sick twice?
Even if Dr. Ackerly's patient is already reinfected with coronavirus, this does not mean that anyone with the infection can have the same fate.
"There are some cases of people getting sick from the Coronavirus twice, but is this the rule or the exception?" Immunologist Menno van Zelm of Monash University said.
Dr. van Zelmsaid infection is possible based on what we know about other coronaviruses, but we don't have the full picture.
In particular, he said, we don't know how many people are exposed to the coronavirus again without getting sick.
If we can set up an experiment to test each person who has recovered from the coronavirus and then intentionally re-expose the virus to find out how many people have contracted the disease, we will know exactly how common the disease is twice.
But of course, this is not an option, so we must trust the reports.
People who recover from COVID and then re-expose themselves to the virus, but don't get sick, don't make headlines like Dr. Akerli's patient.
In fact, they won't necessarily know they've been rediscovered, especially since many people with coronaviruses are asymptomatic.
"It is a difficult issue because we only have a partial view of the virus and we do not know if the [reinfection] reports provide a biased view," Dr van Zelm said.
What we need now is the results of long-term scientific studies that analyze the immune response of large numbers of people over time to find out what happens when they become infected again, Dr. Labzin said.
Stuart Tangye, an immunologist at the Garvan Institute for Medical Research, agreed that there was not enough strong evidence and that we did not know enough about the conditions surrounding the case reports again.
For example, did the patients have pre-existing health conditions, including immune defects, that could make them more susceptible to infection?
"If they do that, it will be an exception, not the rule," said Professor Tangy.
Could a second infection cause a worse disease than the first?
Dr. Labzin said a process called "antibody-dependent enhancement" could lead to a disease worse than a second infection.
This was observed with dengue but has not yet been confirmed to have occurred with COVID-19.
"This [process] is rare and not well understood, and it is one of the things we are studying," said Dr. Labzin.
She said it is important to understand if the process occurred at COVID-19 so that we can design vaccines to avoid this possibility or define new treatments to address them.
But if you do become infected again, the hope is that your immune system's ability to "remember" viruses will result in milder disease the second time.
"From what we know now and from animal studies with SARS-CoV-2, it seems likely that even if people do become infected again, most of them will not necessarily have worse symptoms," said Dr. Labzin.
What does reinfection mean for herd immunity?
Although how immune function works against coronavirus is still largely unknown, Dr. Labzin said the evidence so far indicates that it may not last long.
Recent findings suggesting that antibodies to the virus may disappear rapidly have raised concerns that this may be the case, although it is still too early to know what this means for immunity.
And even if the infection doesn't make us sick again, if we can still pass the virus on to others, this undermines the development of herd immunity.
Dr van Zelmsaid's multiple exposures to the virus may be necessary to develop immunity that stops the infection and transmits the virus.
That is why many vaccination programs provide improved vaccines, he said.
Source: abc.net.au
Also Read: Paytm to launch stockbroking services in the next few weeks: Vijay Shekhar Sharma
POPULAR POSTS
How a Free AI Visibility Tool Helps Businesses Grow in the AI Driven Search Era
by Aakash Ladha , 2026-03-06 10:40:04
Loan EMIs to Drop as RBI Slashes Repo Rate - Full MPC December 2025 Highlights
by Shan, 2025-12-05 11:49:44
Zoho Mail vs Gmail (2025): Which Email Platform Is Best for Businesses, Startups, and Students?
by Shan, 2025-10-09 12:17:26
PM Modi Launches GST Bachat Utsav: Lower Taxes, More Savings for Every Indian Household
by Shan, 2025-09-24 12:20:59
$100K H-1B Visa Fee Explained: Trump’s New Rule, Clarifications & Impact on Indian Tech Workers
by Shan, 2025-09-22 10:11:03
India-US Trade Deal Soon? Chief US Negotiator Arrives in Delhi as Talks Set to Begin Tomorrow
by Shan, 2025-09-15 11:54:28
Modi Meets Xi: Trump’s Tariffs, Strategic Autonomy, and the Future of Asia’s Power Balance
by Shan, 2025-09-03 06:40:06
RECENTLY PUBLISHED

Pine Labs IPO 2025: Listing Date, Grey Market Premium, and Expert Outlook
- by Shan, 2025-11-05 09:57:07

The Agentic Revolution: Why Salesforce Is Betting Its Future on AI Agents
- by Shan, 2025-11-05 10:29:23

Top 10 Insurance Companies in India 2026: Life, Health, and General Insurance Leaders Explained
- by Shan, 2025-10-30 10:06:42

OpenAI Offers ChatGPT Go Free in India: What’s Behind This Big AI Giveaway?
- by Shan, 2025-10-28 12:19:11

Best Silver Investment Platforms for 2025: From CFDs to Digital Vaults Explained
- by Shan, 2025-10-23 12:22:46




 Subscribe now
Subscribe now 